Trudy Townsend on Trauma, the Nervous System, and Creating Safety at the 2026 Facilitation Lab Summit
Trudy Townsend closed out the 2026 Facilitation Lab Summit with a session that went, in her words, “straight at” the topic every other presenter had been circling. After two days of deep work on presence, belonging, voice, and the edges of facilitation practice, Trudy brought the science: why trauma is present in every room a facilitator enters, what it looks like when it surfaces, and what it actually takes to create the conditions where people can show up whole.
Trauma Is Already in the Room
Trudy opened by noting that trauma does not need to be introduced into a facilitated space. It is already there. To make that concrete, she walked the room through the ACEs study, one of the most consequential pieces of public health research of the past 30 years. Conducted in the 1990s by Dr. Robert Anda of the CDC and Dr. Vincent Felitti of Kaiser Permanente, the study asked 17,500 patients to answer 10 questions about adversity experienced before age 18, covering abuse, neglect, household dysfunction, domestic violence, and other forms of harm. The findings were striking: two-thirds of the population had experienced at least one significant childhood adversity. With an ACEs score of four or more, risk for major diseases was substantially elevated. With a score of six or more, life expectancy was shortened by 20 years.

Trudy was clear that this was just the childhood data. Adults keep experiencing things. And the reason it matters so much for facilitators is the same mechanism that made her opening meditation work: the brain pathways that bring comfort and safety are the same pathways activated by traumatic experience. A scent, a facial expression, a tone of voice, a pattern of behavior in a group can all trigger a response that has nothing to do with what is happening in the room right now, and everything to do with what has happened before.
Her definition of trauma was also worth holding: “Trauma is not the event. It is the experience of that event living in your body. It is what happens inside of us as a result of what happens to us.”
Reading the Nervous System
To explain why this matters in practice, Trudy walked the room through Dan Siegel’s hand model of the brain. The thumb tucked against the palm represents the limbic system, anchored by the amygdala, the hippocampus, and the hypothalamus. The amygdala scans constantly for threat and safety. The hippocampus cross-references what it senses against a quick-reference library of past experience, looking for what is familiar. When something registers as significant, the hypothalamus triggers the body’s protective response, flooding the system with hormones. The fingers folded over the thumb represent the prefrontal cortex, where learning, reasoning, and creativity live. When the protective response fires, the prefrontal cortex essentially shuts down. Facilitators have a phrase for this: someone has flipped their lid.
What makes this especially relevant for facilitation is that people with significant trauma histories often walk around in a state of chronic hypervigilance, already partway toward that threshold. They do not signal this. But they do show signs, and part of becoming a more trauma-informed facilitator is developing the ability to notice them. The room surfaced a wide range, including clenched jaws, elevated breathing, redness in the face, crossed arms and averted eyes, sudden withdrawal or silence, nervous laughter, anxious over-participation, thought spirals, and humor used as deflection. One participant offered a crucial caveat: we often do not know what a behavior means. Someone crying might be angry, not distressed. The practice is not diagnosis. It is noticing.
One participant named something the room needed to hear directly: that when we talk about physical safety, we are sometimes talking about different things. For some people in the room, physical safety was genuinely at stake in ways that go beyond room layout or uncomfortable chairs. The conversation did not flinch from that. And Trudy wove it into her central point: trauma-informed practice requires holding the full range of what people carry when they walk through the door.
Safety Is the Antidote
The fundamental antidote to trauma, Trudy argued, is not comfort. It is safety. When the nervous system begins to register safety, the protective response quiets. The jaw loosens. The breath changes. The prefrontal cortex comes back online. Curiosity returns. And with curiosity comes the possibility of learning, of relationship, of productive disagreement.

Trudy named five types of safety she pays attention to as a facilitator: physical safety (freedom from bodily threat), psychological safety (freedom to voice thoughts and opinions), social safety (belonging with the people in the room), moral safety (freedom to do the right thing), and cultural safety (freedom to express one’s true identity and beliefs). Participants worked through table conversations about what builds each type of safety in their practice, and what erodes it.What emerged was practically rich. Physical safety includes room layout, scheduled breaks, sensory considerations, and accessibility. Psychological safety is shaped by how a facilitator responds to contributions, including the ones that do not receive enthusiastic affirmation. One participant named that saying “I love that” in response to some contributions and not others is itself a signal that people will notice and feel. Grounding the voice, slowing the pace, and naming what is happening in the room all contribute to co-regulation. Social and moral safety connect to how clearly shared values and agreements are established, and whether the group is invited to create them rather than simply receive them. And several participants pushed for replacing “safe space” with “brave space,” recognizing that a facilitator cannot guarantee safety but can invite people to commit to bravery together.
Trudy closed with the thread that had run through the entire session: trauma-informed facilitation is not a checklist. It is the sum of everything the summit had been exploring over two days. Showing up regulated. Noticing before interpreting. Preparing well. Asking people what they need before the session begins. Attending to power and agency, because trauma almost always involves a loss of both. And trusting that when people feel genuinely safe, something opens in the room that no technique alone can create.
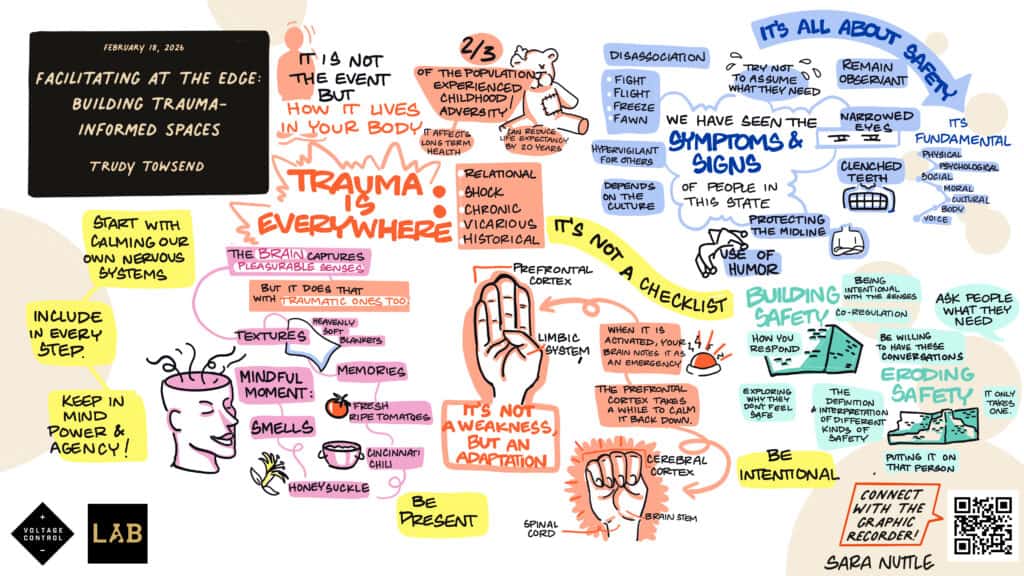
Watch the full video below:
Transcript of Trudy’s Session:
Trudy Townsend:
Y’all, what an incredible couple of days. Wow. Thank you for staying for this. I really appreciate it. I know several of you have flights to catch. I have a flight to catch too, so I get it. If you need to get up and leave, I totally understand. I’m not going to be crushed or anything, but thanks for being here to the very end. I just want to acknowledge that we have been holding a lot over the last couple of days. Our brains are full. Our hearts are full. We’ve been doing a whole lot of touchy-feely stuff.
We’ve been sort of pushing ourselves to those edges and that’s a lot. And I just want to acknowledge that. Thank you. They keep telling me it has to be higher and that’s hard for me. Yeah. Thank you all for being such an incredible audience. From every presenter has told me what an incredible audience you are to work with. So thank you for that. And thank you for the hard work you’ve been doing at Getting to Your Edges. As I start, I know that Dan shared some sort of guiding principles. Does it have to be turned on?
No, I don’t know. Dan shared some guiding principles and I want to share some ground rules too. If my slide starts working, that’d be great. But if not, that’s okay. As we get started, I just wanted to share these couple of ground rules. Every other presenter has really danced around exactly what I’m going to talk about today. And I’ve loved it. Thank you all for setting me up so well. But what I’m going to do is go straight at this topic. And some of you have much more expertise in this topic than I do.
For some of you, this topic is really, really difficult. And for some of you, you can’t wait for me to get started. But I really want you to take what fits, what seems to be great. If I say something that doesn’t jive with you, just let it go. Just leave it. Y’all have been such an incredible audience to just go with the flow, and I so appreciate that. I really do. I really want to ask you to do some deep reflection today. And as you do that deep reflection, I also want you to maintain your own safety. So you’re invited to participate with me. I would love it if you do. And if you can’t, that’s okay too. I get it.
As we broach this topic that I’m probably scaring you all about, please try to care for one another, but also care for yourself. If you need to get up, whatever you need to do is okay. And it’s always okay to just pass. You don’t have to share, but you guys are great at it, so that’s amazing. It’s the end of the day, and you guys have been amazing, but I really want to start with yet another mindful moment. Can we do it? Are we able to do it one more time? One more time, one more mindful moment. It’s really going to help set up my talk, so I appreciate that.
I also just want to acknowledge that for some of us, these mindful moments are so Zen and amazing and incredible. And for some of us, an incredibly quiet mind, closing our eyes, sitting next to someone who is very still is scary. And I get that. So if you’re one of those people where it’s kind of scary to have a quiet mind, I’m going to tell you a little trick. If you just gaze down at your feet and let your body be still for a minute, everybody will think you’re doing it.
So if you really don’t want to do it, that’s cool. No problem. So I’d like to start with this mindful moment, and if you will, just get comfy in your chair. Just get comfy. It really helps if you sort of settle into the chair, maybe push yourself to the back of the chair, let the chair support you. Sometimes it helps if your feet are flat on the ground. And often when we’re mindful, we just start by noticing our breath. You don’t have to change your breath. Just notice the inhale and the exhale. Your body already knows how to breathe, so you don’t have to fix it.
There’s no right or wrong way to do it. Just notice your breath. Now, I’m going to invite you to bring to mind a scent, a smell. Doesn’t have to be a strong one, not an intense one. Just maybe something that feels pleasant, comforting, familiar. Some of us lost our sense of scent or smell during COVID. So if that’s not a great doorway for you, you’re welcome to choose a sound, an image, a place. You get to choose. You don’t have to name it. You don’t have to picture it perfectly. Just let something come to you.
As you hold that scent or sound or image, notice what, if anything, comes with it. Maybe it’s a place, a season, a person, or a feeling, whatever it is. If nothing has come, that’s okay. No need to force it. As this moment kind of concludes, I would just welcome you to come gently back to the room. Maybe start to feel the chair underneath you, supporting you, feel your feet on the ground. And when you’re ready, come back to me. Open your eyes.
Oh, thanks everybody. That calmed my nervous system. I appreciate it. Is there anybody who would like to share what came to them in that moment? You don’t have to tell the whole story, but is anybody willing to share maybe the scent or feeling that you had?
Speaker 2:
I thought of wet earth, the smell of wet earth and vine ripened tomatoes, which my grandmother used to grow in our backyard and I used to eat them off the egg, whole tomatoes. And it just always brings me back to a place of getting safe and loved and grounded.
Trudy Townsend:
And also, there’s nothing better than a garden ripe tomato.
Speaker 2:
Oh yeah. Yeah.
Trudy Townsend:
I love that. I love that. Anyone else?
Speaker 3:
I thought about Cincinnati chili. For folks who don’t know is like clothes and chocolates and all spice. And thought about watching the Super Bowl with family and sort of comfort.
Trudy Townsend:
Oh, I love that. Give me some Fritos and chili anytime. Yeah.
Speaker 4:
So I thought of honeysuckle. It could be the beautiful weather, starting to make summer plans, but honeysuckle goes from my childhood even to now and all the places we love to visit. It reminds me of my close friends I grew up with that I’m still in touch with. It reminds me of moments with my child. I just love it.
Trudy Townsend:
Oh, I love that. We have honeysuckle on our ranch and when you’re riding a four-wheeler and you drive right by that, ugh, that’s a great smell. I love that.
Speaker 5:
So I actually didn’t think of a smell. I am a texture person.
Trudy Townsend:
I love that.
Speaker 5:
So I thought of the … There’s this blanket called the Lola blanket and it is the softest thing on the planet. Think bunny ears velvet. It’s worth every penny. It’s not cheap. I’ve discovered it at a friend’s house. She got it for Christmas. And as soon as she let me touch it, I like dove right in. I head first into this blanket. I’m not even joking. And then my friends were laughing and I was like, “Oh my God, what is this blanket?” It’s the best heaven feeling that I can think of. So I don’t get any points for this, but lola blankets if you’re interested.
Trudy Townsend:
I love that. Love it. Earlier yesterday, it was yesterday, I heard somebody, I think from this region of the room, say, “Wow, our brains are really incredible,” and they are. Just a moment of bringing a scent or a texture or a picture to mind and boom, we’re somewhere else in a different time, in a different place, just completely somewhere else in our mind. It’s really, truly incredible. I wish that I was a Dan. I wish that I was a Brian or a Chris and could just really practice mindfulness all the time because it’s incredible. My mind’s frenetic and so it’s hard for me to do, but our minds are brilliant.
The thing about our brains though is these same pathways that bring us comfort, that bring us familiarity, they’re the same neuro pathways that also work for traumatic experiences. And that’s why trauma is so pervasive. It’s in every single group that you walk into. It’s in the room already. Didn’t have to do anything to put it there, even though sometimes I try my best. And it shows up. No matter what we’re doing, it shows up. It shows up not always in words, but it always shows up in nervous systems. And it shows up in how the group engages.
How many of you have heard of the ACEs study? Raise your hands. This group is so informed. I’m loving it. Love, love, love it. This is really funny. I am probably one of the least nerdiest people I know, but I’m going to spend a few minutes talking about data and some science. There’s a couple of you who don’t know about ACEs, and I love it when I’m the first one that gets to tell you about ACEs. When I’m talking about trauma, I think it’s so important to mention this really groundbreaking study.
So the ACEs study was done in the 1990s, and Dr. Robert Anda from the CDC and Dr. Vincent Felitti, who worked for Kaiser Permanente partnered up to do this study. And they had 17,500 participants who were patients of Kaiser Permanente answer a 10 question survey. These 10 questions were about adversity that the patients had experienced in childhood before the age of 18. The questions were about whether the person
had suffered abuse or neglect, whether they were made to feel loved or special as a child, if their basic needs were met.
There were questions about household chaos and dysfunction, divorce, domestic violence, living with somebody who has a mental health condition or maybe who was incarcerated. So that’s what the questions kind of were. And the way that the ACEs study worked is if that happened to you in childhood, whether it happened once or repeatedly, you marked a one. So you could have an ACEs score from 1 to 10.
And what they found was astonishing. They found that two-thirds … so if you look next to you, the people on either side of you, two-thirds of the population had experienced at least one significant childhood adversity in their lives. Then I think what’s really incredible about this study is it was Kaiser Permanente. So they took that data and they compared it with adult health outcomes. And what they found feels a little devastating to me, but what they found was that there was a dose response between adversity you had experienced in childhood and poor health outcomes as an adult.
With an ACEs score of four or more, your risk of heart disease, cancer, emphysema, many of the top diseases we see in the world were highly elevated. And with a score of six or more, your life expectancy was cut by 20 years. Now, this is incredibly depressing and I understand that. Also, you might think it was the 90s. I’m not going to tell y’all what I was doing in the 90s because I like to think the Botox is working. I live in that sort of world, but if you’re worried about that, these questions have been added to all kinds of public health health risk assessment surveys. They’ve been added to birth of state population health surveys, and the results have been crazy consistent over time.
What this study tells me, and the whole point I want you to take home, is that this matters a lot. Childhood adversity, they’ve also found that chronic stress, living in chronic stress and toxic stress, impact your brain in the exact same way that trauma impacts your brain. It leaves a lasting imprint. I also want to mention, holy smokes, this is just what happened to you in childhood. We’re a bunch of grown up people. Stuff keeps happening. I got hit in the eye with a pickleball like two weeks ago. I went to play pickleball again and I was like, “It was hard.”
Stuff happens and it impacts us and that’s important. And when I think about this and I think about how incredible the brain is that we just think about a scent, we just think about it, bring it to mind and all of a sudden we’re in a different place. What that tells me is every time somebody sees a facial expression, look in my eye, I think about my son when I take a deep breath in front of him. They’re getting a message, some kind of message. And I don’t know what that message is, right? But they’re getting some kind of message. And that’s why this is so important to us as we walk into rooms.
So let’s talk about this word trauma just a little bit more. I always like to level set on what it is. When I first came to understand and learn about trauma, and by the way, I’m not a mental health professional. I’m just a regular person who learned a lot about this. But when I first came to understand it, we were talking about trauma as an event. What we’ve come to understand now is that trauma is not the event. Yes, something happened to you, but trauma is the experience of that event living in your body.
It’s what happens inside of us as a result of what happens to us. And there’s all kind of different ways you can … Pathways to get to trauma. These are just a few of the types of trauma that we experience across our lives. Shock trauma, that’s like the car accident, the crazy weather events we have these days, that big fire ranch I talked about, ranch, fire, whatever it is. Those are shock traumas, things that happen and sort of out of the blue and shift your worldview or your experience. Relational trauma is the one that most people think of because hurt people hurt people.
Relational trauma is that trauma that happens when you think you’re in a safe relationship and it’s not so safe. So it’s abuse, neglect, the lack of psychological safety. That’s relational trauma. Seriously, chronic stress, toxic stress. Some of us just live in it all day long, every day. It’s bad for you. Vicarious trauma, that’s one that’s a little bit hard to understand, but a lot of caregivers get vicarious trauma. It’s often called secondary trauma as well.
So this is something that didn’t happen to you. It happened to somebody else, but you’ve heard about it maybe so often that now it has shifted your worldview, shifted the way that you think about things. So that’s vicarious trauma. And then there’s historical trauma. There’s this science called epigenetics, which I can’t even talk about it because I’m not that smart. But epigenetics shows us that trauma can live in our bodies for up to two generations.
So what happens to me if I don’t deal with it, happens to my kids and my grandkids. I don’t have any yet. Remember the Botox. So all of these are different doorways. These are not all the doorways. Lots and lots of stuff can happen to us across our life, but we come at it from all different experiences. All of them shape how our nervous system learns to protect us. And that protection is the key word because this trauma, it’s not weakness in the system. It’s literally an adaptation of our system. It is what is keeping us alive.
So we have talked and talked about this. Many of my colleagues have mentioned nervous systems. You as facilitators know this intuitively, but I wanted to really share exactly how it works. Some of you know this better than I do, but I’m going to try to run through it with you all using this hand model of the brain. So a really smart guy named Dan Siegel. Anybody heard of the hand model of the brain? Oh, lots of you. Yeah. So when I get it wrong, help me out. So Dan Siegel came up with this hand model of the brain, and I like it because I think it’s just such a good and easy way to remember this. So if you put your hand up in the air, you can do it or not do it, whatever you want to do. We’re looking sort of at a model of the brain, right?
So this right here is your spinal cord coming up into the base of your skull here. I’m sorry about this. The base of your skull, that’s your brain stem right there. And if you take your thumb and just tuck it in like that, your thumb represents a very small but very powerful region of your brain. This is our limbic system and the limbic system is made up of the amygdala. You all want to say amygdala with me because it’s just such a fun word to say. Amygdala. Yeah. Yeah. The amygdala, the hippocampus, and the hypothalamus. Those are the little organs within the brain.
So the amygdala is our central hub for emotions. It’s crucial at forming and consolidating memories and associating them with feelings or emotions. That amygdala, it’s busy. It’s constantly scanning the environment all the time, looking for cues of safety, looking for threat. That’s what the amygdala is doing. And when the amygdala senses something, anything, it immediately, really quickly, in nanoseconds, sends it to the hippocampus. The hippocampus converts it into short-term memories. They convert short-term memories into long-term ones. And I like to think of it as our quick reference library. So I always think of, I think of this little guy up in my brain just running through the files really, really, really quick, like AI, just running, running really quickly through it. And our brain’s like what’s familiar.
So whatever is going on, that facial expression, a smell, whatever it is, the hippocampus is like, “Woo, I know that. I know what that is. I know how we should feel when I see that.” So that’s the hippocampus. And when the amygdala and the hippocampus sense something really important that’s vital, it sends that message right to the hypothalamus. And the hypothalamus is connected to our nervous system. And the hypothalamus is like, “Oh, I got to do something. I got to protect.”
And all of a sudden, hormones start coursing through my body and releasing all of those things so that I can protect myself. Now it takes really quickly to do that, but it’s a real long time before I’m able to kind of cover that up, shut that down, regulate myself with my prefrontal cortex. So this is your prefrontal cortex. Your prefrontal cortex is really important. It’s where you learn. It’s where you think. It’s where you create reason, right? But when this whole thing is going on, the prefrontal cortex literally shuts off.
And that’s when we say people have flipped their lids, right? So if you flip your lid before your prefrontal cortex can kind of come back online, that looks all kind of different ways and groups. So unfortunately for us as facilitators, people don’t kind of walk around with their hands showing us, right? And people who have experienced lots and lots and lots of trauma, or even maybe just trauma in groups, they walk around in a state of hyper-vigilance and that kind of looks like this, right? They’re right on the edge. They’re ready to flip their lid at any moment because they’re already halfway there.
So when you think about that and you think about two-thirds of the population have experienced trauma in childhood, and the rest of us sure got it as adults, this is happening everywhere we go, and nobody’s walking around showing us where they’re at, unfortunately, although we have started to teach children to do it. But you know what? There are signs. There are signs that it’s happening when we’re facilitating. There are physical signs, right? So think about that system, what’s happening in that system when those cortisol and other hormones get released, right? I get hot. My husband calls it hot mad.
So I get really hot. I sweat when I eat cinnamon bears, so it really happens quickly for me. People’s face get a little red. Sometimes their breathing elevates, but there’s lots of physical signs. There’s emotional and psychological signs. People do all kinds of different things, right? Get quiet, get loud, shut down, all kinds of different emotional signs that we see in rooms, and there’s behavioral signs. People fidget, people get up and down, all kinds of things, right?
We’ve seen this in rooms over and over again. You’ve seen this in rooms. And if we can get really good at seeing this in rooms, we can get really good at calming nervous systems. So what I’d love for you to do is just on your own … I’m going to give you two or three minutes, not a very long time, on your own, I’d love for you to just jot down a couple of the signs and symptoms that you’ve noticed when you’re in groups. Some of you have been facilitating forever and you have all kinds of stories in your head about this. For others of you, it might Might be meetings that you’ve been in or one-on-one conversations or family groups. But what I’d love for you to do is jot down one or two symptoms, three or four symptoms, however many you can think of, in each of these categories.
What were some of the physical signs you’ve noticed? What were some emotional or psychological signs that you’ve noticed or behavioral signs? What we’re looking to get at is what do we notice in rooms when nervous systems are dysregulated? How will we know that’s happening? So I’m going to give you a couple minutes. After that, I would love for you to be able to discuss this at your tables. Remember, when you’re writing stuff down and reflecting to yourself, be as open and honest with yourself in those reflections as you can. You only have to share what’s safe.
Okay. Hopefully you have come up with a couple of signs or symptoms. I’d love for you to share those at your table. Just talk together about the kinds of signs and symptoms you’ve seen. All right. Who has a physical sign or symptom that you want to share? By the way, huge shout out to Katie and Mark. Katie and Mark, thank you so much. They have made this possible. Thank you. Who has a physical sign or symptom they want to share? Come on, you all have not been shy. Right behind you, Katie.
Speaker 6:
I had clenched teeth or narrowed eyes.
Trudy Townsend:
Yeah. Yeah. Oh my goodness. That just is me. I just clenched my teeth like this so much and so many people do. Also in our neck, right? That response is muscle tension and it happens so quickly. Thank you for that one. That’s such a good one. Yeah, back here.
Speaker 7:
I’ve heard kind of a bundle of the emotional responses. It’s all being related to protecting the midline. It’s like a very animalistic. So it’s the averting the eyes, crossing the arms, leaning back, and it’s kind of protecting your face and your center body. It’s like-
Trudy Townsend:
Very Right.
Speaker 7:
… the same way you react to any kind of threat, like it’s a physical threat, even if it’s not.
Trudy Townsend:
1,000% because it’s about survival. Such good insight. Thank you for that.
Speaker 8:
I struggle with this a little bit because I’m unsure if I actually know what any signs or symptoms actually mean, unless I actually explore and ask them what it means.
Trudy Townsend:
Right.
Speaker 8:
Because someone could be crying. I think you have an example of a person, a story was shared with me where a person in facilitation was crying and people were really trying to console and help. And then there was a moment where she was like, “Stop. I’m not upset. I don’t need anyone to hold me. I’m actually angry and I’m processing.” So there was an automatic assumption that people knew what the person was experiencing based on a particular behavior or emotion. So yeah, that’s kind of where I am.
Trudy Townsend:
I really love you bringing that up because you’re right. We don’t know. We’ve all been experiencing these two days, every single one of us. And my experience is super different than your experience, right? Some of us are like loving this. Some of us are like, “I got to go home now.” Right? This is about, we don’t necessarily have to know exactly what to do. All we have to do is notice somebody’s experiencing something, right? And as facilitators, that’s what we’re doing. We are fine-tuning our noticing skills, right? That’s what we’re doing. As we interact with groups, we’re noticing. How about emotional? Over here. Wow, you’re ready.
Speaker 9:
Yeah. For me, I tend to overthink a lot of things. I feel like my brain is overloaded with too many thoughts and I would also go into thought spirals, overthink a lot of things.
Trudy Townsend:
Yeah, absolutely. We all have that over thinker in our groups, don’t we? And sometimes overthinking is so hard because your brain’s going so fast and then somebody asks you a question and you’re like, it can look like dissociation. It can look blank. We see those blank faces. And back to your point over there, that’s not a bad thing. You’re diving into whatever we’re doing, right? You’re thinking it through, you’re overthinking it. It’s not bad. There’s nothing I need to do, but I might notice, right? As a facilitator, I might notice that and maybe think, “I should slow down or not.” Yeah. Really, thank you for that. Anybody else? An emotional sign or symptom? Psychological sign or symptom? I know that can be hard. Yeah.
Speaker 10:
Just based on what you shared right now, the thing that came to mind was hyper-vigilance. You mentioned it earlier. Yeah. I think hyper-vigilance can be a sign of maybe some of us that had to be caregivers very early on in our lives. And so we enter teams and we feel like we need to emotionally support everybody and in a large capacity and so a sign of that could be always kind of being hypervigilant. Is this person being included? Is this other person being listened to? And that can be a sign of that.
Trudy Townsend:
I so appreciate that you brought that up. I failed to mention earlier, it’s all about that fight, flight, freeze. What you’re talking about is fawn, right? That need to take care all the time, that need to people please, that need to overdo that, right? That is also a nervous system response. So thank you for bringing that up. Appreciate that. It gets really heavy, doesn’t it? Back here in the very back. Mark, thanks.
Speaker 11:
I think it’s interesting because it’s really about content as well, right? So being a facilitator requires us to pay attention to individuals as they’re coming in the room because everyone and all these physical, emotional responses are so different in every single person. And so when I see this in X person, it might not mean anything. But if you’re noticing something that’s out of the ordinary, then it becomes the sign that’s showing you.
And that’s the, “Hey, let’s pause. I noticed this.” And it’s giving yourself enough grace to be that observer from the beginning because we don’t know and no one’s going to tell you, “Hey, nice to meet you. I have some trauma and this is what I’m going to give you. So please pay attention to this for the next 20 minutes.” So that’s the part of how do we continue to scan the room, sculpt the room, to look for, again, not something that may be obvious to us, but it’s out of the ordinary for maybe that person.
Trudy Townsend:
I really appreciate that. And what you said made me think of another really important point, you and you. Guess what? It’s not just the participant because when you notice something, you’re having a response too, right? And you’re thinking some kind of way that could be totally not the thing, right? But we still need to notice because it is out of the ordinary for the group or for that person, right? So thank you for bringing that up. Appreciate you. Ooh.
Speaker 11:
Got it.
Trudy Townsend:
Over here and then to you, Joe, and then we’ll move on.
Speaker 12:
I think one of the things we need to keep in mind too is sometimes what will show up will depend on the culture.
Trudy Townsend:
I love that. I heard you talking about that back there.
Speaker 12:
So in North America, we’re often a guilt and consequence culture, Western, right? But a lot of my friends who are from Asia are much more of a shame, honor culture. And then other people I work with are a power, fear culture. And so how it shows up will depend on the culture that you’re dealing with and working with.
Trudy Townsend:
So important to talk about. We’re going to talk more about that later. Thank you for that. Joe, and then we’ll try to move on.
Joe:
Yeah. I was just going to mention one that has prompted a lot of reflection for me is humor and how nervous laughter or sort of attempts to redirect conversations always to somewhere humorous triggers for me a series of exchanges and that’s sort of how you respond to them, that it’s something that generally is a positive thing. And so you may give back to it, but in the spirit of what others have said, you don’t know whether it’s sincere humor, whether it’s reflection of something deeper. And so humor is one that to me particularly is complicated to navigate.
Trudy Townsend:
I so appreciate that. I was talking to Brian earlier. He was talking about how much he uses dad jokes, right? And a lot of people, we use all different kind of protection mechanisms. I have another girlfriend that whenever you go to any party with her, she is the show. And I love it because then I don’t have to be the show, but that is a fear response. That’s okay. I love it. I eat it up. That’s great. And I know she needs to be that person. And that’s great.
So thank you for that. It’s true. It shows up in all kinds of different ways. What do you think is the one thing in all these scenarios, whether we know what’s happening or not, what is the one thing that people need when we’re activated, when our nervous system gets activated? What do we need? Anybody got a guess?
Speaker 14:
Awareness.
Trudy Townsend:
Awareness? We as facilitators sure need awareness, right? What do they need when their nervous system is activated?
Speaker 14:
[inaudible 00:41:26].
Trudy Townsend:
Right. What she said is co-regulation.
Speaker 14:
Like a co-regulation.
Trudy Townsend:
Girl, you are working it. Thank you. Yeah. Co-regulation.
Speaker 14:
Attunement of some kind from another human in some way, maybe.
Trudy Townsend:
Yeah. I think what people are looking for is safety because our nervous systems are trying to protect us, right? They’re really trying to get to a place of safety. Listen, this isn’t bad. This is good. It keeps us alive, right? Our nervous system is so important to our survival. It was built for the dark ages where we are running from tigers. So the nervous system is good, but what it is seeking is safety. So safety is a fundamental antidote to trauma. It’s not being more comfortable. It’s not that one person in every room who complains about the temperature that I can’t do anything about.
It’s safety because when the nervous system calms down, lets the prefrontal cortex kick in, it starts to register safety. We naturally shift out of protection mode. Our breath changes. Our jaw loosens. Muscles start to soften. Our attention widens when we feel safe. We’re able to return to curiosity. We’re able to use our words. So safety is what makes learning possible. It’s what makes relationship possible. It’s what makes engagement happen. And it’s what makes conflict workable. For safe, we can engage. We can disagree. If we’re not safe, it’s hard to do that.
Here’s the deal though. There’s not just one type of safety. If you Google safety, guess what? You’re going to get a lot of hard hats. Okay. So there’s not just one type of safety. There’s lots of different types of safety. These are the ones I pay the most attention to when I am facilitating. So physical safety. Are we safe in our body, safe from physical threat? Psychological safety. Are we safe with our thoughts? Do we feel safe enough to voice our thoughts and opinions? Social safety. Do I feel safe with the people at my table? With the people in this room? I feel really safe with this group. You guys are amazing.
And then I feel like I can’t say this one enough in the groups that we’re facilitating. Moral safety. Do I feel safe enough to do the right thing? Cultural safety. Thank you so much for bringing that up. Do I feel safe enough to express my true self, my true beliefs? All right, y’all. Let’s make this real. You guys are professionals. So what I would love for you to do right now, first of all, I need a volunteer at each table. Can you raise your hand if you’re willing to volunteer? One volunteer for each table. Looking at each table? Awesome. Thank you so much.
Your job is not hard. What I’m going to ask you to do is I’m just going to ask you to start the conversation and I’m also going to ask you to make sure that you’re clicking through each type of safety. Okay? So keep the conversation going. We’re not going to have a long conversation. We’re going to have about a seven-minute conversation. But what I want you to do at your tables is I want you to talk through how you, as a facilitator, what are the strategies you use to build physical safety?
What do you do in your planning processes throughout the day? How do you build physical safety for your groups? How do you build psychological safety for your groups? What do you do as a facilitator? How do you make psychological safety happen? Social safety, moral safety, cultural safety. Move through that list and just engage in conversation with one another, sharing the strategies that you use to build safety in the rooms you’re in for each of these types of safety. Okay? Seven minutes, table facilitators. Awesome.
Okay. Are y’all back? Back? Those were good conversations. Really good conversations. This is a talented room. So I’m going to take a couple from each category. There’s a lot of categories. So physical safety. What are some things that you all do as facilitators? What are the choices you make? Conditions that build safety. Got it.
Speaker 10:
So physical safety was one that we initially started talking about … not really sure how to word it, but we dove deeper into it and we thought about intentionally scheduling breaks, making sure that we could, when we’re meeting with people, we asked them about their energy levels, giving them a heads-up that a break was coming up, even going more deeply into also the smells of the shared space, understanding that some people might be more sensitive to smell and that might affect their experience in the moment, making sure that there’s enough chairs so everybody is comfortable. So exploring the idea of comfort and safety together.
Trudy Townsend:
I love that you brought in the senses. That’s beautiful. Thank you so much. Let’s take one more condition that builds safety.
Speaker 4:
Adding to those. We also talked about location and room layout and things like that, that truly physical to the room that might fit that conversation you’re trying to have.
Trudy Townsend:
I love that. I think also where people are at in the room is important, right? Maybe making sure you’re spreading out the power dynamics a little bit across the room. Really good. What are some conditions that erode safety in groups? You don’t have to tell me big stories, but maybe something that you know that really erodes physical safety.
Speaker 11:
It only takes one.
Speaker 6:
I was just going to say, we had uncomfortable chairs at one point and there was different … Just people who were very uncomfortable in certain chairs. And we also were one time at a school that the elevator was not working. And so people who had mobility struggles to get to the second floor of a building that was like right from the very start of the day, put people off in their physical safety.
Trudy Townsend:
Absolutely. What about activities that require physical movement? Yeah. One here, one over there.
Speaker 14:
I was going to say that … Oh, sorry. I was going to say that everybody must stand and stay standing the whole time. I’ve been in workshops where people have done that.
Trudy Townsend:
Yeah. Yeah.
Speaker 14:
You don’t know what people’s issues are.
Trudy Townsend:
Right. Right.
Speaker 15:
I just, in terms of the elephant in the room, wanted to hold some space for the fact that truly there are some bodies that are not safe. There are some of our colleagues here who are more likely to get rounded up than others. There are some of us who have a historical trauma and some of us who don’t, and it feels like we’re not really talking about safety. And if you’re someone like me and I have to look at my students and say, “Here’s what will happen if someone comes to round you up.” When I have to look at trans faculty and say, “Okay, if they will not let you use your passport, you do not have to go to this thing.”
The physical safety that we’re metaphorically talking about, I just want to say to the people who might not actually be physically safe, I would love for us to talk about actual unsafety, people who are being oppressed physically, women, gender violence. When we talk about bodies being traumatized, I think we’re really talking about survivors of sexual violence, right? So I just want to ground for a second for people who might be sitting like I am going like, “I don’t know if we’re all talking about the same safety.”
An uncomfortable chair is not physical unsafety. That’s a lovely way to talk about safety, but I just want to be sure that if you’re sitting there going like, “Yeah, I just don’t want to get rounded up. I’m hearing you.” And I would love for people to think about those things too. Sorry.
Trudy Townsend:
No, I really appreciate that. Thank you for bringing that into the space so much. There is such a rainbow of things because experiences live in our body, fear lives in our body. So thanks for bringing that up. There is a wide, wide list of things that are our responsibility as a facilitator, no matter what we’re facilitating. We’re facilitating programs, we’re facilitating sessions. So thank you for that. Let’s talk about psychological safety because that matters too, right? Are we safe enough to be here? Yeah. What are some things that we do as facilitators that build safety?
Renita:
I think one thing that we talked about and I was identifying myself of how I maybe inadvertently losing safety is how I’m responding to people’s comments and questions. I’m a very much like, if someone says something, “I love that. I love that.” Then I’m thinking about for the comment that I don’t say I love that.
Trudy Townsend:
Yeah.
Renita:
How is that person now like, “Well, wait, was my comment not valid?” And I just didn’t want to keep overusing. So now I’m trying to find other neutral language of acknowledgement that also doesn’t sound like a robot of like, “Thank you for sharing, thank you for sharing, thank you for sharing.” So making sure there’s like a balance of how I am responding to the group because that evokes all types of trauma and validation and work, all the things that are there.
And then even to the point of making sure my voice is grounded in moments of activation too, because I know that in my past I’ve gotten activated by voices. I’m like, “Oh, you sound like my mom yelling at me.” And so when things get activated, I drop my register down and I slow my tone so that it can co-regulate the group too. So all those little subtle dynamics are alive.
Trudy Townsend:
Using those mirror neurons to help co-regulate with others. Thank you so much too for raising how we interact with groups is really vital to safety. So thank you for that, Renita. Yeah, over here.
Speaker 17:
We talked about the importance of kind of like naming the gaps and when we fail to embody our values and what we say we believe, just to level set and also like create room for that to be acknowledged and maybe ideate on what could that look like if we’re not embodying it, how could it be?
Trudy Townsend:
Yeah. Yeah. That’s beautiful. So much of what we’ve talked about over the last two days really are about how do we show up? How do we demonstrate those values? How do we generate the conditions in the room? Yeah.
Speaker 18:
This is something that I definitely bring into the facilitation practice, but I’ve learned outside of the facilitation practice, which is when you’re in a company of rowdy people, say people who might have drunk too much as well. I remember being at a barbecue once in the mountains in this place in central Italy, and it was like a bike spot and I was brought in by a group of bikers. They were super nice, but they definitely drank too much. They had too much to drink.
And so there was the feeling of the edge was kind of ready to flip. And I had this conversation with one of them who had drunk a little bit less than the others, and he said, “Well, the trick here is just to treat them like gentlemen.” And I was like, “Okay, let’s try it.” And the response was perfect. I mean, they were on edge, but they were like, “Oh yeah, I’m a gentleman. Yeah.” I will stay gentlemenly throughout. And so that’s something I also bring into my facilitation practice by giving people a chance to be generators of safety, psychological safety.
Trudy Townsend:
I love that. You bring up something that I think is vital to safety and that’s respect. People need to be respected in order to feel safe. So thank you for that. Yeah.
Speaker 8:
One here.
Speaker 19:
As facilitators, we all say these catchphrases like, “Let’s create a psychologically safe space or this is a judgment free zone.” Well, we can’t guarantee a psychologically safe space. We can’t guarantee a judgment free zone either. So one thing you said, one thing my group talked about was you had an example is that you say, “Let’s create a brave space.” And would you explain to us what you meant by that?
Speaker 20:
Yeah, this is not my work. If you do a search for a brave space, there’s an awesome quote that goes over it in more detail, but the gist is basically, to that point, we can’t guarantee that something that said is going to make someone not feel safe, but we can all, as part of our agreements, is agree to be brave and to be brave to have these tough conversations.
Trudy Townsend:
I love that. That’s a great reframe. Hi, Dan.
Dan:
Hey. Yeah, I think too, I [inaudible 00:57:20] arrival, just splashed everything everywhere. Yeah, I think part of this we’ve talked a lot about in the session and what we do in that moment, but I also think there’s that piece prior to the session too, how we’re building that awareness together. I find too, we place the burden on the person who’s experiencing the traumatic event and the challenges.
Trudy Townsend:
Right. Point them out.
Dan:
Yeah. Say I’m not. And how do we share that as a collective burden amongst the group so that we can name it too? I think that’s another important piece that I’ve seen work really well.
Trudy Townsend:
Yeah. Yeah. Renita.
Renita:
Sorry. I’m not sorry. I have things to say. But I want to build on what Dan said, because it just brought to my attention something that’s worked in the past, and I’m going to do a Monday as I’m crafting this session, is for people to stop and think about, write down what you need to be safe. I think we are proactively trying to create these things, but people individually haven’t thought like, “Well, I feel safe when, and these are the conditions that I need,” versus, “Well, I don’t feel safe. Well, why?” “Well, I don’t know why. Well, let’s actually take some time to see what safety looks like for you or for what trust looks like.” So that way they can also have a way of taking care of themselves and that can be built into the collective agreements that Dan was also just was talking about too, so letting people have time to think through it.
Trudy Townsend:
I love that. I was running out of time, so I skipped over this. Can I see my slides again really quick? Flynn, like the lights. Oh, good. Renita has taught me so much about interviewing clients, talking with clients, the pre-work with clients. I skipped over this exercise, which was probably a wrong facilitator move, but I mean, maybe we could ask these questions, right? Maybe we could actually ask people what they need.
What I really want to tell you is that trauma-informed care isn’t a list of things, right? It’s not a checklist you can do. It is all the things we’ve talked about over the last two days. It’s being present. It’s understanding the signs and symptoms. It’s preparing well. It’s showing up regulated, whatever that looks like for you. It’s noticing all day long, pre, mid, Post. That’s what trauma informed care is. And all of us are already doing some form of this.
We’re already doing it. But if we can train ourselves to get better at spotting the cues, if we can train ourselves to get better in the interview phase, to get better in the prep phase, to pay more attention to the world around us, what is happening for the people I’m about to encounter? What feels safe for them? What doesn’t feel safe for them? What is their culture? What is their beliefs about safety? If we can get really good at that part, think about the incredible engagement. If I’m safe to engage in a conflict with someone who has more power than me, just think about how we can change the dynamic, change what happens in the world. But in order to do that, we have to access our prefrontal cortex.
We can’t walk around with our lids flipped all the time. It also really matters for us as facilitators to figure out how to regulate in that moment. So it’s noticing ourselves. I love all of this mindfulness stuff that we did. I love the sensing stuff, the embodiment stuff. Not all of us are really good at that. I wish I was better at it. But if we can work on fine tuning those systems within ourselves, creating habits for ourselves, we can get even better at this. Thank you for putting up with my sort of nerdiness. I didn’t get to everything, which is just me. I never get to everything.
Thank you for doing this with me. Thanks for stretching to this kind of hard edge at the very end of a very long two days. I appreciate you more than you know. I am kind of at time, right? 4:30? Yeah. Well, you told me 4:30, buddy. So anyways, oh, I had this whole bit about power. You guys understand that … I just want to say this one more thing. Power matters because when people are traumatized, usually it involves a loss of power, a loss of agency, a loss of control.
So when you’re thinking about those power dynamics, that’s important. It’s really important. And so it’s not only about safety, it’s also about agency. So much about agency. So you guys are already doing this. You know what you’re doing. Let’s just get better at it and better at it. Okay. So I’m going to get to here.
And what I would love for you to do is think about a strategy that you heard at your table. Think about one thing that you’re going to get better at. Put that up on the board. Thank you so much to the whole desk in the back that’s making all this happen. Amazing. Thank you to this incredibly talented graphic recorder. Thank you to the volunteers. We’re going to create brave spaces. We’re going to be more vulnerable. We’re going to think about acknowledging safety. I’m going to regulate myself. I love this, y’all. Thank you so much. Thanks for letting me be here.


